ESR News June 2014
Are Diagnostic X-rays Safe for Pregnant Patients?
John Damilakis, Professor of Medical Physics
Whenever a diagnostic or interventional X-ray examination of a pregnant patient is considered to be necessary, embryo/foetus dose estimation is an essential step in assessing the radiogenic risks to the unborn child. Accurate estimation of embryo/foetus radiation dose is also needed after accidental exposure of a pregnant patient from an X-ray procedure. When the uterus is remote from the directly exposed anatomical area, the embryo/foetus is exposed to scattered radiation and its dose is negligible (dose lower than 1 mGy). Normally, a detailed embryo/foetus dose evaluation is not needed for such studies. Radiological examinations involving the abdomen or pelvis may deliver relatively high radiation dose to the unborn child. For abdominal examinations, maternal body size and uterus position should be taken into consideration to obtain accurate dose estimation. Patient-specific Monte Carlo simulations have been used to accurately estimate radiation dose from an abdominal CT examination (Figure). A standard CT examination for appendicitis or ureteral stones performed on the mother would result in an embryo/foetus dose of about 25 mGy. Multi-phase abdominal CT examinations may deliver relatively high doses to the unborn child. Doses to the unborn child below 100 mGy should not be considered a reason for therapeutic abortion. The risk to the embryo/foetus for stochastic effects is assessed on the basis of radiation dose using appropriate risk factors. Although these risks from a single diagnostic procedure are low for the vast majority of diagnostic X-ray examinations, it is important to ensure that radiation doses to the mother and child are kept as low as reasonably achievable.
There has been a substantial increase in the use of imaging procedures with ionising radiation during pregnancy in the US (Lazarus et al, Utilization of imaging in pregnant patients: 10-year review of 5270 examinations in 3285 patients, Radiology 251:517-24, 2009). The utilisation of radiologic imaging in pregnant patients is lower in Europe. Furthermore, accidental irradiation of pregnant patients during the first post-conception weeks leads to unnecessary termination of pregnancies. As part of the CONCERT project, a survey was implemented in Greece to evaluate current practice patterns in imaging of pregnant patients and examine policies for screening women of childbearing age for pregnancy before radiological procedures. A large sample of radiologists, interventional cardiologists, medical physicists and obstetricians covering a wide geographical area of Greece was targeted through four online questionnaires. Recipients of the questionnaires were asked about hospital and department demographics; departmental policies on imaging the pregnant patient; number of ionising radiation examinations performed on pregnant patients; written informed consent obtained before imaging with ionizing radiation; radiation protection measures during exposure of pregnant patients; availability of radiation protection garments; pregnancy screening of adolescents and women before radiologic procedures; and frequency of accidental exposures. The main conclusion of this study was that the utilisation of radiological imaging in pregnant patients is very low in Greece. On the other hand, cases of accidental irradiation of pregnant patients during the first post-conception weeks are not rare. Clear recommendations are needed for management of pregnant patients needing radiological procedures.
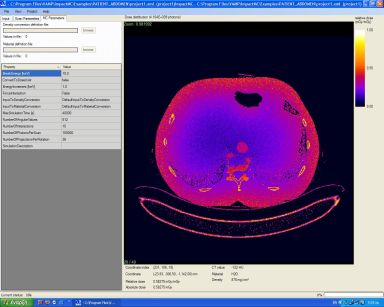
Figure. Monte Carlo software packages can be used to a) develop voxelised models based on image data from patients who underwent MDCT examinations and b) calculate patient-specific radiation doses. Each pixel in the image represents a radiation dose value. Black indicates the lowest dose, whereas white indicates the highest dose.